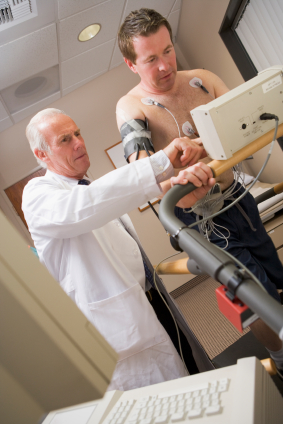
Healthy non-diabetics making the switch to the paleo diet rarely, if ever, experience hypoglycemia. That’s not true for diabetics, especially if they’re on certain medications.

Hypoglycemia now would be a tad inconvenient
Hypoglycemia means an abnormally low blood sugar (under 60–70 mg/dl or 3.33–3.89 mmol/l) associated with symptoms such as weakness, malaise, anxiety, irritability, shaking, sweating, hunger, fast heart rate, blurry vision, difficulty concentrating, or dizziness. Symptoms often start suddenly and without obvious explanation. If not recognized and treated, hypoglycemia can lead to incoordination, altered mental status (fuzzy thinking, disorientation, confusion, odd behavior, lethargy), loss of consciousness, seizures, and even death (rare).
You can imagine the consequences if you develop fuzzy thinking or lose consciousness while driving a car, operating dangerous machinery, or scuba diving.
Do not assume your sugar is low every time you feel a little hungry, weak, or anxious. Use your home glucose monitor for confirmation when able.
Why Would the Paleo Diet Cause Hypoglycemia?
Carbohydrates are the the primary source of blood glucose (blood sugar). Paleo diets typically derive anywhere from 20 to 40% of total calories from carbohydrate, with 30% being about average. This compares with 50-60% of calories coming from carbs in the usual American diet. Additionally, the overall glycemic index of paleo diet carbs is likely to be lower than an average American diet since there are no refined starches and sugars. A lower glycemic index tends to limit blood sugar spikes in response to a meal. So any diabetic switching to a paleo diet could see significant drops in blood sugar, including hypoglycemia.
How Is Hypoglycemia Treated?
If you have diabetes, your personal physician and other healthcare team members should teach you how to recognize and manage hypoglycemia. Immediate early stage treatment involves ingestion of glucose as the preferred treatment—15 to 20 grams. You can get glucose tablets or paste at your local pharmacy without a prescription. Other carbohydrates will also work: six fl oz (180 ml) sweetened fruit juice, 12 fl oz (360 ml) milk, four tsp (20 ml) table sugar mixed in water, four fl oz (120 ml) soda pop, candy, etc. Fifteen to 30 grams of glucose or other carbohydrate should do the trick. Hypoglycemic symptoms respond within 20 minutes.

Lady, fruit juice would raise your blood sugar much quicker
If level of consciousness is diminished such that the person cannot safely swallow, he’ll need a glucagon injection. Non-medical people can be trained to give the injection under the skin or into a muscle. Ask your doctor if you’re at risk for severe hypoglycemia. If so, ask him for a prescription so you can get an emergency glucagon kit from a pharmacy.
Hypoglycemia Unawareness
Some people with diabetes, particularly after having the condition for many years, lose the ability to detect hypoglycemia just by the way they feel. This “hypoglycemia unawareness” is obviously more dangerous than being able to detect and treat hypoglycemia early on. Blood sugar levels may continue to fall and reach a life-threatening degree. Hypoglycemia unawareness can be caused by impairment of the nervous system (autonomic neuropathy) or by beta blocker drugs prescribed for high blood pressure or heart disease. People with hypoglycemia unawareness need to check blood sugars more frequently, particularly if driving a car or operating dangerous machinery.
OK, the Acute Crisis Is Over — What Next?
If you do experience hypoglycemia, discuss management options with your doctor: downward medication adjustment, shifting meal quantities or times, adjustment of exercise routine, eating more carbohydrates, etc. If you’re trying to lose weight or control high blood sugars, reducing certain diabetic drugs makes more sense than eating more carbs. Eating at regular intervals three or four times daily may help prevent hypoglycemia. Spreading carbohydrate consumption evenly throughout the day may help. Someone most active during daylight hours as opposed to nighttime will generally do better eating carbs at breakfast and lunch rather than concentrating them at bedtime.
DRUG ADJUSTMENTS TO AVOID HYPOGLYCEMIA
Hypoglycemia is a great risk for diabetics taking certain diabetic drugs while on a low-carb paleo diet. This is dangerous territory.
Remember, drugs have both generic and brand names. The names vary from country to country, as well as by manufacturer. You’ve got to know what class of drug you’re taking. If you have any doubt about whether your diabetic drug has the potential to cause hypoglycemia, ask your physician or pharmacist.

That’s the ticket
DRUGS THAT CAUSE HYPOGLYCEMIA
Regardless of diet, diabetics are at risk for hypoglycemia if they use the following drug classes. Also listed are a few of the individual drugs in some classes:
- insulin
- sulfonylureas: glipizide, glyburide, glimiperide, chlorpropamide, acetohexamide, tolbutamide
- meglitinides: repaglinide, nateglinide
- pramlintide plus insulin
- exenatide plus sulfonylurea
- possibly thiazolidinediones: pioglitazone, rosiglitazone
- possibly bromocriptine
DRUGS THAT RARELY, IF EVER, CAUSE HYPOGLYCEMIA
Diabetics not being treated with pills or insulin rarely need to worry about hypoglycemia. That’s true also for prediabetics.
Similarly, diabetics treated only with diet, metformin, colesevalam, and/or an alpha-glucosidase inhibitor (acarbose, miglitol) should not have much, if any, trouble with hypoglycemia. The DPP4-inhibitors (sitagliptan and saxagliptin) do not seem to cause low glucose levels, whether used alone or combined with metformin or a thiazoladinedione.
Thiazolidinediones by themselves cause hypoglycemia in only 1 to 3% of users, but might cause a higher percentage in people on a reduced calorie diet. Bromocriptine may slightly increase the risk of hypoglycemia.
DRUG ADJUSTMENTS TO AVOID HYPOGLYCEMIA
Diabetics considering or following a carbohydrate-restricted diet must work closely with their personal physician, dietitian, or certified diabetes educator, especially to avoid hypoglycemia caused by the aforementioned classes of diabetic drugs.
Clinical experience with thousands of patients has led to generally accepted guidelines that help avoid hypoglycemia in diabetics on medications.
Common strategies for diabetics on hypoglycemia-inducing drugs and starting a low-carb diet include:
- reduce the insulin dose by a quarter or half
- change short-acting insulin to long-acting (such as glargine)
- stop the sulfonylurea, or reduce dose by a quarter or half
- reduce the thiazolidinedione by up to a half
- stop the meglitinide, or reduce the dose by up to a half
- monitor blood sugars frequently, such as four times daily, at least until a stable pattern is established
- spread carbohydrate consumption evenly throughout the day
Management also includes frequent monitoring of glucose levels with a home glucose monitor, often four to six times daily. Common measurement times are before meals and at bedtime. It may be helpful to occasionally wake at 3 AM and check a sugar level. To see the effect of a particular food or meal on glucose level, check it one or two hours after eating. Keep a record. When eating patterns are stable, and blood sugar levels are reasonable and stable, monitoring can be done less often. When food consumption or exercise habits change significantly, check sugar levels more often.
No One Cares About Your Health As Much As You
I recommend you become the expert on the diabetic drugs you take. Don’t depend solely on your physician. Do research at reliable sources and keep written notes. With a little effort, you could quickly surpass your doctor’s knowledge of your specific drugs. What are the side effects? How common are they? How soon do they work? Any interactions with other drugs? What’s the right dose, and how often can it be changed? Do you need blood tests to monitor for toxicity? How often? Who absolutely should not take this drug? Along with everything else your doctor has to keep up with, he prescribes about a hundred drugs on a regular basis. You only have to learn about two or three. It could save your life.
If you’re thinking that many diabetics on low-carb diets use fewer diabetic medications, you’re right. That’s probably a good thing since the long-term side effects of many of the drugs we use are unknown. Remember Rezulin (troglitazone)? Introduced in 1997, it was pulled off the U.S. market in 2001 because of fatal liver toxicity. In 2010, rosiglitazone was heavily restricted in the U.S. out of concern for heart toxicity.
Steve Parker, M.D.

![MP900178842[1]](https://paleodiabetic.com/wp-content/uploads/2012/02/mp9001788421.jpg?w=300&h=201)